What is Fibromyalgia?
Fibro Active
What is Fibromyalgia: Unraveling the Symptoms
Fibromyalgia (FM or Fibro) symptoms are part of a syndrome of symptoms that are common and overlap other illnesses including Chronic Fatigue Syndrome (CFS)/ME, Depression and Anxiety, Rheumatoid Arthritis, Lupus, Irlen Syndrome, MS, Raynaud’s and many more. Sometimes it can be difficult to identify one illness from another.
Fibro is only one part of an extended list of concurring symptoms that occur in the syndrome, but also has an extended list of symptoms that often coincide with one another.
What causes Fibromyalgia?
Fibro Active do not promote the use of medication for Fibromyalgia and are not GP’s therefore unable to recommend medication especially with the complications of side effects, taking meds for other conditions and we all react differently. You should never take another person’s medication and always consult your GP before you try any promising ‘miracle cure!’ That being said Fibro Active do have a team of specialists that can help you manage your pain and symptoms using gentle exercise, nutrition and lifestyle advice and emotional support.
This is not a new illness!
Although Fibro was only recognised as a real chronic illness in 1990, it has been noted by various well-known people. Ironically by Hippocrates over 2000 years ago but also Florence Nightingale, a local Derbyshire nurse, whose birthday we celebrate as International Fibromyalgia Awareness Day on May 12 th . More recently well-known faces have included: Morgan Freeman and Sinead O’Connor along with Lady Gaga.
Fibromyalgia is now a recognised illness
Moreover, after all these years of sufferers being told it was in our heads. Fibromyalgia was officially recognised on October 1st, 2015 and now has an official diagnosis code M79.7. Still to this day some older medical practitioner’s do believe it is all in our heads. It is advisable if you have this experience to see a younger doctor who would have been taught about this in their training.
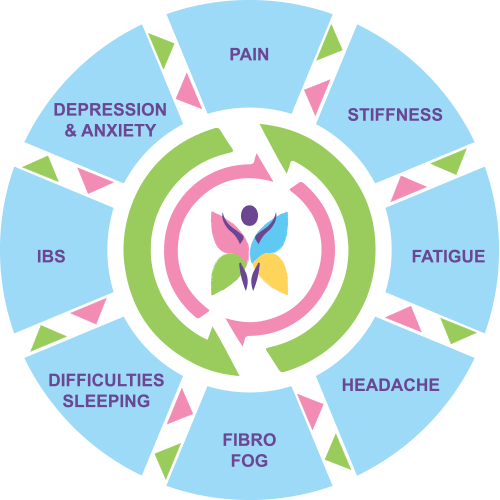
What are the symptoms of Fibromyalgia?
Fibromyalgia is a complex condition known for its diverse symptoms, with over 200 identified. These include widespread pain, fatigue, sleep disturbances, and cognitive difficulties (“fibro fog”). This multitude of symptoms underscores the challenge in diagnosing and managing fibromyalgia, emphasizing the necessity for personalized approaches to its treatment.
How do people get Fibromyalgia?
Although many sufferers have been able to trace symptoms back to their childhood, diagnosis for many wasn’t until their 30’s or 40’s. Remember being told you have growing pains? Now you are 35 and you keep telling yourself you have growing pains!
How is Fibromyalgia diagnosed?
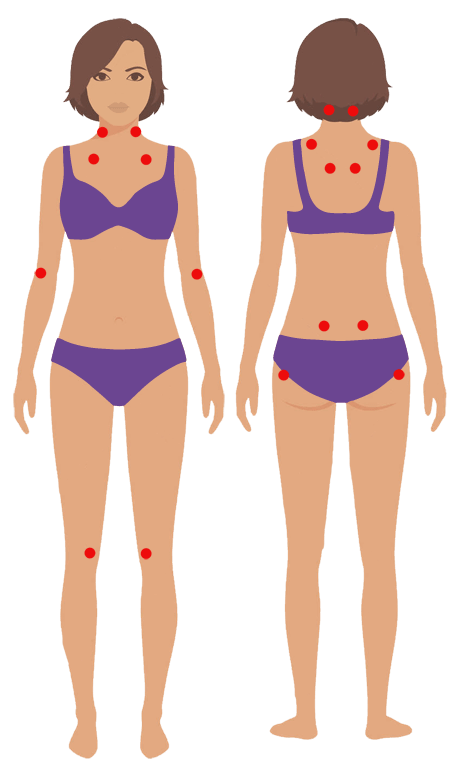
Trigger Points
Trigger points are not to be confused with tender points. Common areas of trigger points include the head and back of the neck, the main joints of the legs and under the feet.
Trigger points are primarily due to myofascial constriction. Chronic myofascial pain (CMP), also called myofascial pain syndrome, is a painful condition that affects the muscles and the sheath of the tissue called the fascia that surround the muscles. CMP can involve a single muscle or a group of muscles. Trigger points occur over many areas of the body and often in layers.
What is a Flare?
10 Things that Contribute to Fibro Flare
- Weather Changes
- Over-exertion
- Stress
- Illness or injury
- Hormonal changes
- Temperature changes
- Lack of or changes in sleep routine
- Treakment changes
- Travelling
- Individual sensitivies
What are limitations?
Fibro Tip:
Know your limits.
Recognize when your strength is fading and take a break before you hit the wall.
Managing your symptoms
Before proceeding it is essential to make sure you are ready for this! It’s all about where you are at and how you approach this.
There are two ways you can manage your symptoms and these methods subsequently rely heavily on your focused perspective.
One option is to become consumed in depression and absorbed in self-pity, refusing to let yourself have any quality of life, by living in a negative bubble where you are always in chronic pain with a can’t do attitude. Having a good moan does not improve your symptoms it just solidifies them!
The other option you can embrace a new life with fibro and accept that you have this illness. It doesn’t happen overnight but by learning to understand it, is like putting the pieces of a puzzle together. ‘Oh, so that’s why I feel like that’ or ‘that’s why that happened’, will put you in a better place and as you will learn later the lower the mood the greater the symptoms.
We call it PFA – Positive Fibro Attitude!

Give yourself the best quality of life you can have under the circumstances by adapting your lifestyle and reducing your stress. It’s not about fighting the illness it’s about managing it, planning, accepting that a flare day is a recovery day not a setback, understanding the consequences of exceeding your limitations, it’s bite sized steps tiptoeing along so that you don’t awake the ‘alien’ inside you.
The choice is yours!
Celebrating Florence Nightingale’s 200th Birthday in 2020
Florence Nightingale, pioneer statistician and renowned, revolutionay nurse. In a time when nursing was looked down upon, Florence saw it as her calling during her early 20’s. She lead a group of 38 nurses over to the Crimean war, the death toll being high from infection and poor nutrition.
Florence developed a sanitary environment along with an active plan for improved nutrition that resulted in the saving of 1000s of lives. She contracted Crimean Fever at the age of 38 under active duty, sadly from then on she was almost entirely bedridden until she died reaching the age of 90.
Florence was a meticulous note taker, keeping a detailed diary that described the perpetual pain, fatigue and general brain fog that related to an illness of no name. The medically trained of the era would disparagingly refer to it as females hysteria.
Nursing was championed through her the first professional nursing school was established, Florence founded London’s Nightingale School of Nursing the reputation of nursing was raised to profession status through this Her direct influence led to the setting up of the red cross in 1870, Queen victoria awarded her the first Royal Red Cross in 1883.
A woman of great distinction appreadiated by many understood by Fibro and CFS/ME sufferers for what she endured.